|
In 1994, the DSM-IV classified PTSD under Anxiety Disorders. The criteria reflected the view that the symptoms occurred as a result of exposure to a significant stressor, and not due the individual. In the third revision (DSM III, APS, 1980) following the Vietnam War, the term PTSD was introduced for the first time. 48), and the etiology of the symptoms was linked the individual, not the event, as it was believed that “if the patient has good adaptive capacity his symptoms usually recede as the stress diminishes.” (Schubert & Lee, 2009) The DSM-II referred to PTSD-like symptoms as “transient situational disturbance” (p. In 1968 the second DSM was published (DSM-II APA, 1968) and the diagnosis of gross stress reaction was omitted. The main causal factor was listed as stressful environmental events, such as natural disasters or war. American Psychiatric Association, 1952), and what is now known as PTSD was labelled “gross stress reaction”. The first Diagnostic and Statistical Manual of Mental Disorders was published in 1952 (DSM-I 1st ed. John Erichsen also went on to note that it was not a phenomenon exclusive to railway collisions “I will not confine my illustrations to cases drawn from railway accidents only, but will show you that precisely the same effects may result from other and more ordinary injuries of civil life.” (pg 22 Erichsen 1867). Railway collisions were relatively common for the time. One of the earliest recorded scientific presentations about the phenomenon we now know as PTSD was in 1867 where the phenomenon was referred to as ‘Railway Spine’ and outlined as something “sustained by passengers who have been subjected to the violent shock of a railway collision” (pg2 Erichsen 1867). Long before WW1, it is believed that Shakespeare provided historical descriptions of PTSD in his writing, which dates to approximately 1597 (Shay 1994). 
What follows is a brief summary of the changes in the formal psychiatric diagnostic criteria, although long before these criteria existed, people recognised these symptoms as evidenced by how the term shell-shock entered the vernacular following WW1. These differences reflect factors such as socio-cultural and political changes, as well as developments in evidence-based understanding of trauma and its sequalae. Specify if: Chronic: if duration of symptoms is 3 months or more.The diagnosis of PTSD has seen several iterations over the decades. Specify if: Acute: if duration of symptoms is less than 3 months. The disturbance causes clinically significant distress or impairment in relationships with parents, sibling, peers, or other caregivers or with school behavior. The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.į. Duration of the disturbance is more than 1 month.į. Duration of the disturbance (symptoms in criteria B, C, and D) is more than 1 month.Į. 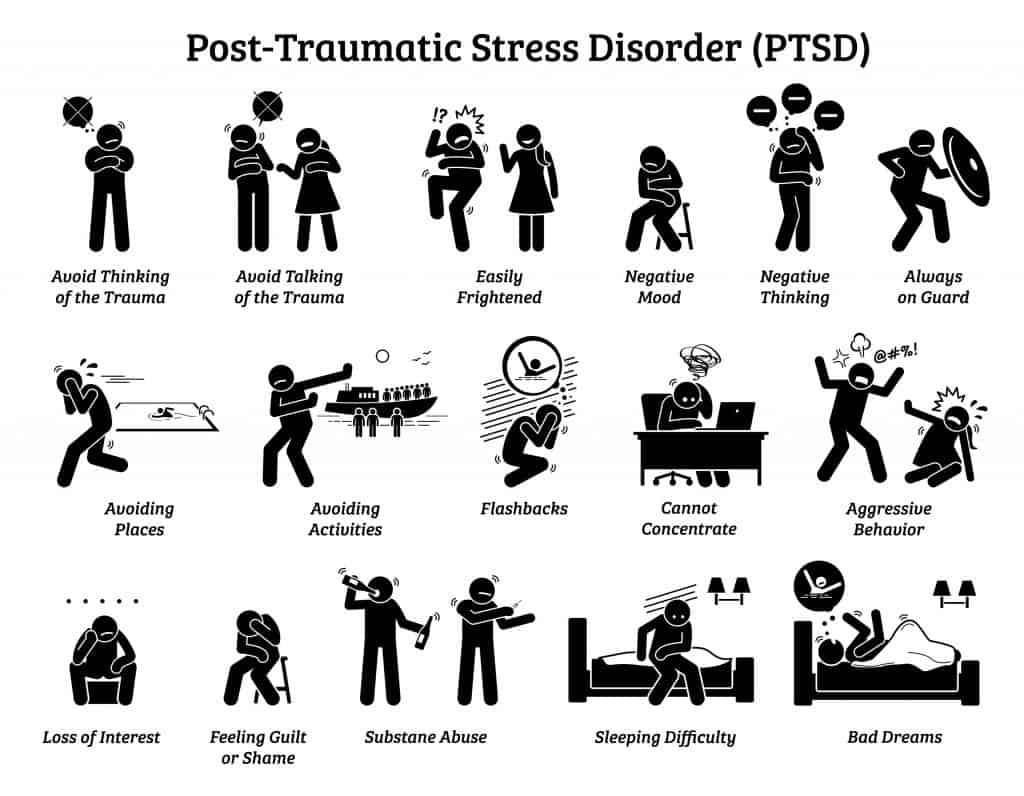
Irritable behavior and angry outbursts (with little or no provocation) typically expressed as verbal or physical aggression toward people or objects (including extreme temper tantrums). 
Sleep disturbance (e.g., difficulty falling or staying asleep or restless sleep). 
Alterations in arousal and reactivity associated with the traumatic event(s), beginning or worsening after the traumatic event(s) occurred, as evidence by two (or more) of the following: 5. Persistent symptoms of increased arousal (not present before the trauma), as indicated by two or more of the following:ĭ. Persistent reduction in expression of positive emotions.ĭ. Markedly diminished interest or participation in significant activities, including constriction play 5. Substantially increased frequency of negative emotional states (e.g., fear, guilt, sadness, shame, confusion). 2.Īvoidance of or efforts to avoid people, conversations, or interpersonal situations that arouse recollections of the traumatic event(s).Negative alterations in cognitions 3. One or more of the following symptoms, representing either persistent avoidance of stimuli associated with the traumatic event(s), or negative alterations in cognitions and mood associated with the traumatic event, must be present, beginning after the traumatic event(s) or worsening after the event.Īvoidance of or efforts to avoid places or physical reminders that arouse recollections of the traumatic event(s). Sense of a foreshortened future (e.g., does not expect to have a career, marriage, children, or a normal life span).Ĭ.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
